In an era of routine air travel and disease multipliers born of human behaviors, a public health crisis anywhere in the world is a potential problem everywhere.
For over one hundred years, nations have negotiated measures to prevent cross-border disease spread. Approaches that endured through the twentieth century focused on protecting international trade and travel by harmonizing the public health measures taken at ports, and on protecting public health through notification procedures for a few specific diseases. Over time, these agreements lost significance as the handful of diseases they addressed faded as threats to global commerce. Traditional regimes had no answer to newly emerging infections such as HIV or to re-emerging infections like multidrug-resistant tuberculosis that spread in more virulent form or to new populations.
In 1995, the Member States of the World Health Organization (WHO) agreed on the need for better disease surveillance and response tools on a global scale. A decade later, in the wake of the international SARS epidemic and the spread of a deadly “bird flu,” WHO’s governing body accepted the dramatically revised International Health Regulations [IHR (2005)].
Transforming international public health cooperation
The IHR (2005) focus on containing public health threats where and when they occur, rather than solely at ports and borders. They emphasize flexible responses to any potential public health emergency of international concern, instead of preset measures for specific diseases. The revised regulations also confer new obligations on countries to report health crises in a timely and transparent way, and new responsibilities and authorities on WHO to coordinate international responses to these crises.
Most significantly, the agreement requires all 194 States Parties to strengthen and maintain core capacities for disease detection, assessment, reporting, and response – capacities that are very uneven worldwide. Countries must develop the legal and regulatory mechanisms, physical infrastructure, human resources, and tools and processes necessary to ensure that all IHR (2005) obligations can be met, all the way down to the community level. This demands long-term cooperation across disciplines and sectors. The revised regulations entered into force in 2007, beginning a two-year planning phase followed by a three-year implementation period. (Nations may request up to two 2-year extensions if they fall short of the 2012 deadline for compliance.)
Building global health security at home and abroad
The U.S. formally accepted the IHR (2005) on 3 December 2006 through an Executive Agreement by the President. Nineteen Federal agencies, led by the Department of Health and Human Services (HHS), worked with the White House to craft the U.S. position during the IHR revision process. Fewer play active roles in implementing the regulations. The HHS Assistant Secretary for Preparedness and Response (ASPR) leads these efforts, coordinating the review, assessment, and notification of potential public health events and promoting domestic implementation and compliance. U.S. disease detection and response capabilities rely heavily on state and local public health capacities. Communications between the state and Federal levels and across sectors remains a serious challenge. Despite these perennial challenges, the U.S. is generally assumed to be well within the requirements for IHR (2005) compliance.
The outlook is less rosy in other regions. The IHR (2005) framework assumes that countries will build their national public health surveillance and response capacities on the foundations of functional health systems. Many weak states fall short of this prerequisite, and a larger number of low and middle income states face solvable but serious gaps. The onus is on national public health leaders to define how they will implement the regulations, and to find the necessary resources. The IHR (2005) created no formal finance mechanism to support implementation. The scope of capacity-building and the lack of defined metrics present a quandary for donors who are uncertain about what it might mean to help partner nations fund IHR compliance.
The global disease detection and response network is only as strong as the weakest link. Article 44 of the revised regulations encourages states to collaborate “to the extent possible” in detecting and responding to health crises, and in sharing technical, logistical, financial, and legal support to help other states implement the IHR (2005). As the largest bilateral donor of health assistance, U.S. leadership and responsibilities in this area are preeminent. The U.S. recently initiated a more robust dialogue among states at various levels of economic development, with the ultimate goal of cultivating IHR (2005) capacity-building partnerships.
Aligning local public health and global biosecurity priorities
Many countries have begun to invest in strong health systems at home and abroad. Reliable public health surveillance lies at the foundation of efficient health systems, and at the core of the IHR (2005). The IHR framework offers the global health community a template for cooperative capacity-building efforts that build local capabilities for evidence-based health policies and reinforce measures to prevent naturally, accidentally, or deliberate released infections from spreading internationally.
This is no guarantee of long-term success. The IHR directly touch on politically charged issues from individual rights to state sovereignty. The legal mandate of the revised regulations may be a tool to empower health ministers within their own governments, but can also be perceived as an unfunded mandate on nations with other health priorities. Building the necessary capacities will require sustained commitment from national leaders inside and beyond the health sector, as well as consistent funding over the long-term.
U.S. agencies – even those that have engaged in capacity-building for decades – will require new strategies to measure progress in building global disease detection and response capabilities. This includes a whole-of-government assistance strategy that breaks down programmatic silos among security, science, and health actors.





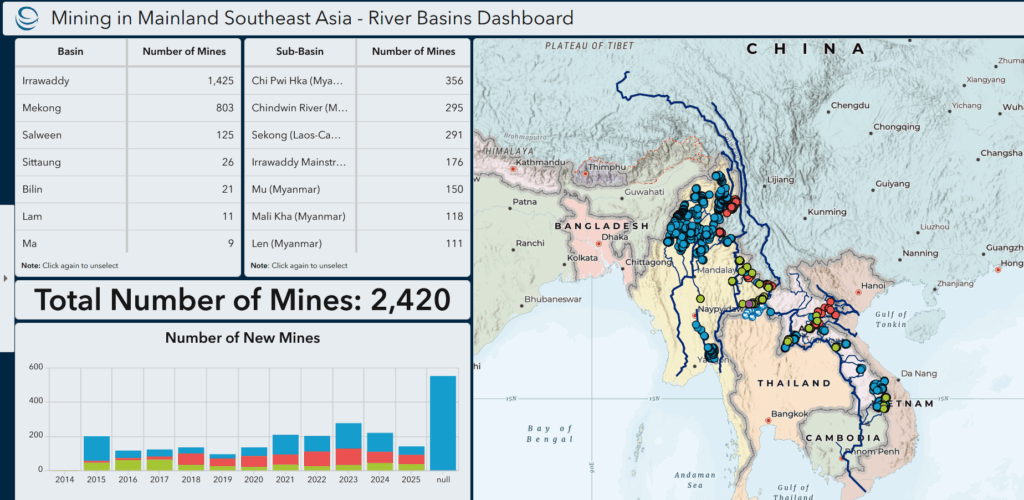


Current Geopolitics Shift Deep-Sea Mining Debates